The subject of medical robots normally accompanies the assumption that they will soon replace clinicians. Those employed in healthcare know a different truth: healthcare embodies the repetitive and risk-heavy work for which robotics was developed. Anyone who has worked in a hospital understands the demand for patient care exceeds the amount of time you have in a day. This combined with ever-present staffing shortages and increasingly sick patients leads to physically demanding work which wears at the human body.
Enter the incredible innovations which have arrived with robotic-assisted surgery. These surgical systems are designed to reduce medical errors, assist surgeons with difficult fine motor tasks, and reduce the repetitive stress which occurs with prolonged surgeries.
A few of these incredible platforms are outlined below.
Da Vinci and Ion – Intuitive Surgical
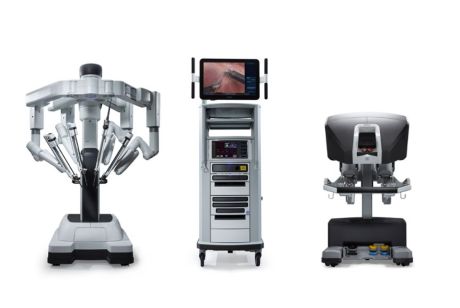
Intuitive Surgical was the first minimally invasive robotic surgery to come to market after being founded in 1995. The da Vinci surgical robot was first cleared by the FDA for general laproscopy, and through the years Intuitive has introduced several different da Vinci systems which allow surgical assistance for complicated procedures with precision and small incisions.
Instruments paired with the da Vinci system include clip appliers, suction and irrigation tools, needle drivers for suturing and closing incisions, and additional tools for dissection, coagulation, and cutting. This diversity in tasks allows a physician not only to perform tasks with precision and accuracy to ensure quality of a procedure, but also addresses healing time by reducing the size of incisions.
Additionally, the Ion system by Intuitive has been introduced and provides a catheter which is able to navigate the peripheral lung space for performing procedures such as biopsies.
Monarch – Auris Health

The Monarch platform provides a flexible, powered system for internal endoscopic procedures such as bronchoscopy. The current indication is to provide visualization and contact with patient airways for diagnosing and treating patients.
The platform is comprised of a robotic systems and its accessories, including a remote-power user interface which allows physicians to control the movement of the endoscope. Ultimately the goal of the platform is to tackle diseases such as lung cancer by providing more efficient and minimally invasive techniques for surgeons.
AquaBeam – PROCEPT BioRobotics

Aquabeam is a robotic water ablation designed for the treatment of BPH (benign prostatic hyperplasia). Like the other systems, Aquabeam provides a combined visualization and treatment system to maximize efficiency and precision in patient care.